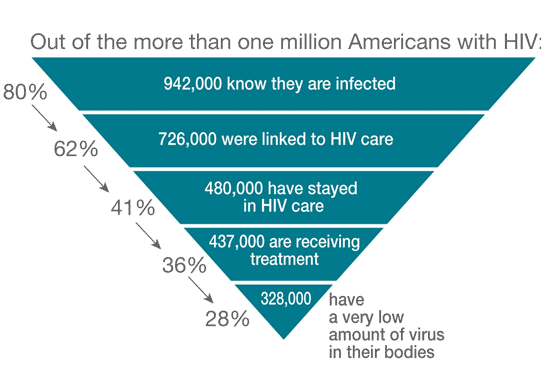
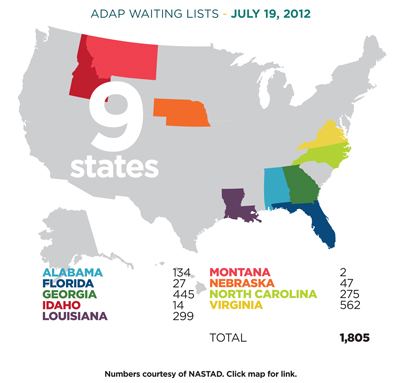
From Jag Davies, Drug Policy Alliance in today’s Huffington Post:
Throughout the world, research has consistently shown that drug criminalization forces people who use drugs away from public health services and into hidden environments where HIV risks become significantly elevated. Mass incarceration of nonviolent drug offenders also plays a major role in spreading the pandemic, as inhumane conditions and lack of HIV prevention or treatment measures in prison lead to HIV outbreaks and AIDS cases behind bars – and among families and communities once those imprisoned are released.
Yet in countries where addiction is treated as a health issue, the fight against HIV/AIDS is being won. New HIV infections in countries such as Australia, Germany and Switzerland have been virtually eliminated among people who use drugs, just as mother-to-child HIV transmission has been eliminated in countries that make medicines for pregnant women accessible.
In the United States, however, the federal government has resisted evidence-based HIV prevention strategies — costing us hundreds of thousands of lives and billions of dollars. Congress re-instated a longstanding ban last December that prohibits using federal funds for syringe access programs — a move that will cost thousands of more lives in years to come.

Money talks- just remind your politicians that the money they are not spending on “immorality” is costing the taxpayers 1000x the amount in the long run…